Trusting the Data to Overcome a Rare Heart Condition

BMC Brighton cardiology patient Danielle Kinney has more energy and less fatigue after successful surgery for a rare heart defect.
The first sign that something was wrong came from Danielle Kinney’s Apple Watch. While hustling through the busy primary care office where she worked, the 49-year-old receptionist and mother of two noticed her watch was showing concerning data.
“It all started last summer,” she begins. “I looked at my watch and noticed that my heart rate was dipping into the 40s. Working in a primary care office gave me the opportunity to share my watch data with a PCP and ask whether I should be concerned about the results.”
Danielle had no prior cardiac concerns—no high cholesterol, no high blood pressure, or anything typically associated with heart disease—but that drop into the 40s, combined with her watch’s year-over-year data, was enough for her PCP’s office to order an electrocardiogram (EKG).
A physical examination revealed a murmur, and though it was “probably something benign,” the provider suggested an echocardiogram or an “echo.” At the time, it didn’t feel urgent, and Danielle didn’t see it as something that needed immediate attention.
“During the echo appointment, I apologized to the tech for even being there,” Danielle recalls. “I couldn’t shake the feeling that someone else needed this slot more than I did, and that I might be taking an opportunity away from someone who truly needed it.”
However, testing revealed that Danielle did in fact need this appointment. An emergency CT scan was scheduled, and the additional test confirmed that Danielle had an incredibly rare congenital heart defect.
How Danielle Came to BMC Brighton
At the time, Danielle didn’t have a cardiologist, making an already overwhelming moment even more uncertain. “My doctor said, ‘You’re going to need a top doctor and potentially a top surgeon,” she shares. “She started to make arrangements, and I just had to trust the process.”
Her PCP coordinated an introduction to BMC Brighton’s Joseph Carrozza, MD—Chief of Cardiovascular Medicine and regularly recognized on Boston Magazine’s Top Doctors list—who would soon take the lead in her care.
Danielle arrived at BMC Brighton, with her husband Steven at her side, to meet with Dr. Carrozza for the first time and make sense of what would come next. “That was probably the most thorough appointment I’ve ever had,” she says. “I must have been in his office for a good 45 minutes while he explained every single piece. I had very few questions because he was just so thorough.”
Dr. Carrozza encouraged Danielle to reach out at any time. He also made it clear that additional research and testing would be needed to fully understand the condition and determine the best path forward.
Her Incredibly Rare Diagnosis
The official diagnosis was a massive right coronary artery aneurysm ending in a fistula—an abnormal connection between blood vessels—which created an unusual pathway for blood flow. Essentially, a high-volume stream of blood was going into a low-pressure area of Danielle’s heart, the coronary sinus. Because the artery was draining into a low-pressure area, it was enlarging her heart, causing a left-to-right shunt.
Normally, a person’s heart sends oxygen-rich blood out to their body, powering organs and muscles. Instead, Danielle’s blood was being rerouted through her lungs and away from the heart muscle, limiting how much reached both sides of her heart. Her heart was working harder than it should have, while her body had less efficient circulation.
Danielle was living with a condition that occurs in only 0.002 percent of the population. Of those, only seven percent have hearts that drain into the coronary sinus. “In 35 years of doing this, I had never seen this,” Dr. Carrozza admits. “Most doctors will never see this.”
Given the complexity of the case, Dr. Carrozza consulted with his colleague and fellow Boston Magazine Top Docs honoree, cardiac surgeon Arvind Agnihotri, MD. From the start, Dr. Agnihotri approached Danielle’s case with a level of preparation that stood out.
“Before I even walked into Dr. Agnihotri’s office, he had already sent over an extensive 30- or 35- page research report on my condition to Dr. Carrozza,” Danielle says. “I hadn’t even met him yet, and he had already dedicated so much effort and time to understanding my case.”

Danielle’s family—husband Steven; their son; and their daughter, who is a nurse—became fully immersed in researching her condition.
A Coordinated Approach to Care
What followed was a series of tests and minor procedures, each of which revealed further insight into Danielle’s condition.
Danielle’s family—husband Steven; their son; and their daughter, who is a nurse—became fully immersed in researching her condition. It quickly became clear that open-heart surgery would be the most viable option, but with so little information available aside from a handful of case studies, the surgical team wouldn’t have a complete understanding until the procedure itself.
“The high blood flow from the fistula made it difficult to do a complete preoperative mapping,” Dr. Agnihotri explains. “We had a general idea of the fistula location, but to properly restore normal circulation, we would need to verify its location during the operation and make sure we had options for different potential locations.”
As her care plan continued to take shape, an unexpected complication briefly interrupted the process. One Sunday night, Danielle noted that her heart was beating unusually. She knew she needed to get to a hospital, but given everything going on, it would be almost impossible to explain everything to an emergency room team. So, despite her guilt for disturbing him on Sunday, Danielle did exactly as Dr. Carrozza told her to do and called him, leaving a message on his personal phone. Within minutes, Dr. Carrozza called back, reassured her that she did the right thing and coordinated with the care team at BMC Brighton for her arrival. “He brought his team up to speed,” Danielle smiles. “He let them know exactly what I needed and just took care of me. While I was there, Dr. Carrozza visited with me, making sure that I was doing well and completely at ease. I’ve never heard of anything like that happening before.”
Because of this, Dr. Carrozza and his team were able to quickly diagnose and treat what turned out to be a heart rhythm disorder, atrial fibrillation (“AFib”), preventing any further complications and keeping their care plans on track.
Making Final Preparations for Surgery
While Danielle had complete trust in the team guiding her care, hearing the details during her final consultation before surgery was still difficult. Her case was complex, with very little precedent. The success of the surgery would depend on carefully reconstructing the abnormal connections in her heart.
“Before meeting Danielle, I spent time reviewing any available information about her condition and how to treat it surgically,” recalls Dr. Agnihotri. “I developed a plan with options, depending on what we found during the operation. When we met, she was very knowledgeable and asked thoughtful questions. She understood my approach and the flexibility needed based on what we might uncover during surgery.”
As part of the conversation, they talked through the potential risks, including the possibility that she might not survive the procedure. For Danielle, the hardest part wasn’t thinking about herself, but how her husband felt hearing that.
Steven remained steady throughout the appointment, but once they reached the parking garage, the emotion caught up with him. “He was so strong, but once we made our way outside, he just folded in my arms and sobbed,” Danielle quietly shares. “Seeing my condition through my family’s eyes was actually harder than experiencing it myself.”
On the day of the procedure, a coordinated, hand-picked team came together for a seven-hour open-heart procedure. For Danielle’s family, it was a long day of waiting. Despite periodic updates, there was a great deal of uncertainty. As a family, they walked through the streets of Brighton, visiting local shops, and stopping for an emotional slice of pizza—trying to distract themselves from what was happening up the block.
Finally, after a long day of waiting, they received the call that the surgery had been a success, and they could see their wife and mother.
From Inside the Operating Room
While the family was waiting, Dr. Agnihotri and his team had been hard at work. The surgical team knew they could find additional concerns that scans hadn’t shown. As predicted, they identified one early—a small patent foramen ovale (PFO), a communication between the right and left atria. While it was not the primary issue, it was repaired as part of the operation.
Addressing the more complicated concerns required far more extensive work. Rather than simply closing the fistula—which would have created a significant risk of clotting—Dr. Agnihotri had to reconstruct the pathway of blood flow entirely. This involved ligating, or tying off, much of the right coronary artery and creating a new route for blood to reach her heart muscle through a triple bypass. Due to her atrial fibrillation, the team also removed the left atrial appendage—where most blood clots form—to help prevent future issues.
“The operation went as well as we had hoped,” Dr. Agnihotri begins. “One of the risks was that we might not fully restore blood flow to the right side of her heart, so it was very encouraging to see strong heart function on her echocardiogram after surgery.” Dr. Carrozza adds, “In a complex case like this, shared decision making with a well-informed patient and a multidisciplinary team led to an excellent outcome.”
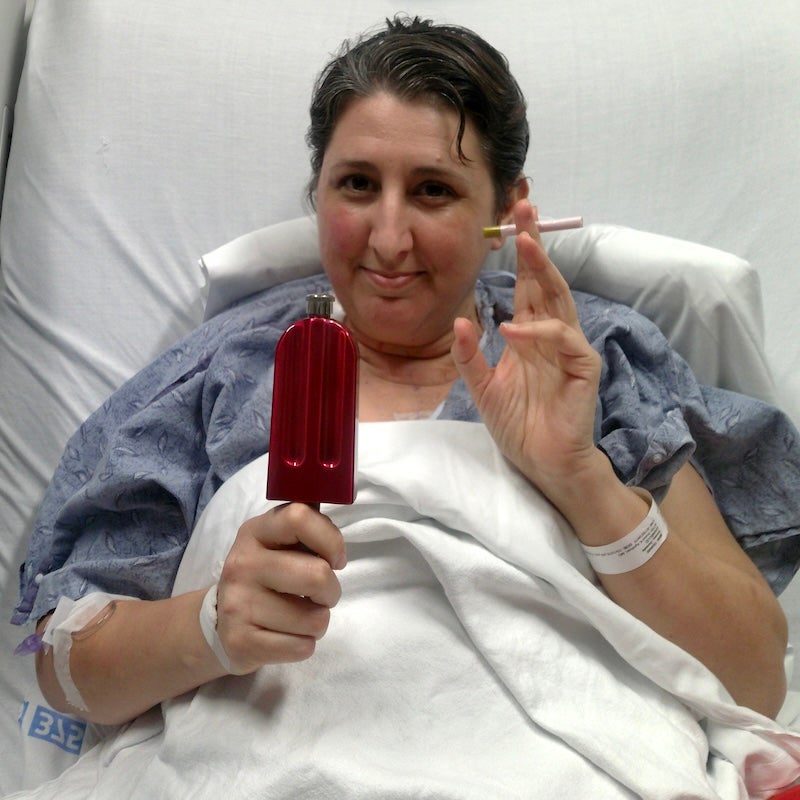
Danielle Kinney has never had a cigarette in her life, but as a joke, she brought in candy cigarettes for the staff, doing her best to make people smile.
Recovering for the People Who Need Her
In total, Danielle spent about nine days in the hospital, moving from the ICU to a regular floor and dealing with physical challenges and side effects. Even in those early moments, Danielle was determined to keep moving. Encouraged by her care team, she was up and walking as soon as she was able—sometimes turning those walks into what she jokingly called her “catwalk,” bringing a sense of humor and lightness to the hospital halls.
“I’ve never smoked a cigarette in my life, but I showed up to the hospital with 24 packs of bubble gum candy cigarettes,” she says with a grin. “I ended up handing them out to the staff, just trying to make people laugh. Humor’s always been how I deal with tough situations, so having these lighthearted moments with the staff made everything feel a little less overwhelming for me. Hopefully it brought them some joy, too.”
For Danielle, recovery was never just about herself. Danielle pushed herself each day, focused on getting home so she could be there to support her daughter through her own medical issue.
When Dr. Agnihotri and Dr. Carrozza came by to check on her, Danielle was often already out walking the halls—miles each day, sometimes with a candy cigarette in hand. “Her recovery was ahead of schedule and without complication,” says Dr. Agnihotri. “I think her positive attitude and energy were unique strengths for her.” That positivity and strength got her home, back to the family who had been there for her every step of the way.
Sharing Her Story with Others
Now, more than four months removed from her surgery, Danielle has had time to reflect on her experience. “If you had asked me at the time, I would have said I was pretty much asymptomatic,” she says. “Because my condition was congenital, it felt like my norm and I didn’t question it, but there were clearly signs I overlooked.”
It wasn’t until after surgery, and through recovery, that overlooked signs became clear. She has more energy, less fatigue, and has even lost weight that had been difficult to manage despite maintaining a healthy lifestyle.
There is also a lasting physical reminder of what she’s been through. “I wake up in the morning and see my chest scar, and honestly, it reminds me how strong and resilient I am,” she says with a bright laugh. “I went through a lot to get here, and now I wear this with pride.”
Her story hasn’t just changed her own life. It has influenced those around her, as friends, loved ones, and even strangers have sought out a cardiologist after hearing her story, many prompted by that one Apple Watch reading. “I have a neighbor who had been an Android user for years, and when she heard my story, she actually bought an iPhone so she could pair it with an Apple Watch,” Danielle says.
Danielle’s intuition ultimately saved her life. By listening to her body when something didn’t feel right, she found the care she needed, and now she hopes others will do the same. “I was asked, ‘Why BMC Brighton? Are you sure they can handle such a complex case?’” Danielle says openly. “I want the community to know that when faced with a medical crisis, you can trust BMC Brighton. The providers at BMC absolutely have the expertise to manage complex cases and, as a patient, you can expect skilled and compassionate care. My rare condition led me to an exceptional care team, and I truly believe that the care I received at BMC Brighton is something I would not have found anywhere else.”
Nationally-Recognized Heart Specialists
BMC Brighton’s Cardiovascular Medicine Department connects you with some of Boston’s top cardiologists, interventional cardiologists, electrophysiologists, and cardiac surgeons, as well as offering advanced treatments for the most complex cardiac conditions from our skilled doctors, nurses, and technicians.
The Center for Advanced Cardiac Surgery offers some of the most advanced procedures available today, including transcatheter aortic valve replacement (TAVR), pulmonary vein isolation, and the Cox MAZE procedure. From complex open-heart operations to minimally invasive techniques, each surgery is performed with a specially trained cardiac surgery team working together to provide comprehensive care before, during, and after surgery. Our dedicated cardiac surgery facilities and team approach ensure seamless care and timely access for patients, families, and referring providers.